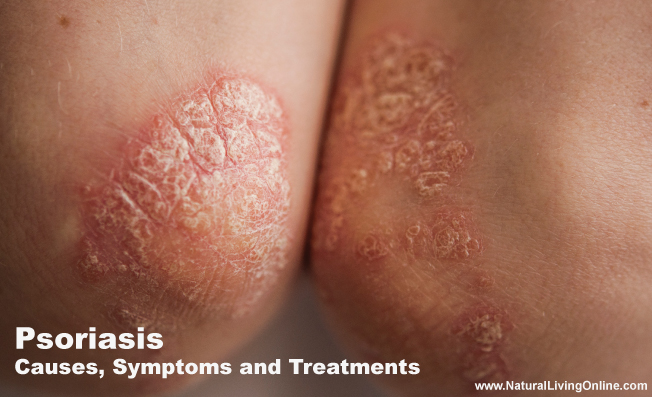
Psoriasis is a chronic autoimmune condition that affects approximately 2-3% of the world’s population. It is a non-contagious disease that causes red, scaly patches on the skin and can also affect the nails and joints. Psoriasis can be a challenging condition to manage and can have a significant impact on an individual’s quality of life.
Causes
The exact cause of psoriasis is not fully understood, but it is believed to be related to an overactive immune system. In individuals with psoriasis, the immune system mistakenly attacks healthy skin cells, leading to the development of the characteristic red, scaly patches. Other factors that can trigger or exacerbate psoriasis include stress, infections, certain medications, and injury to the skin.
Clinical Signs and Symptoms
The hallmark of psoriasis is the development of red, scaly patches on the skin, which can be itchy and painful. The severity of psoriasis can vary from person to person, with some individuals experiencing only mild symptoms while others experience severe symptoms that significantly impact their quality of life.
The clinical signs and symptoms of psoriasis can vary depending on the type of psoriasis, but some common signs and symptoms include:
Red, scaly patches
The most common sign of psoriasis is the development of red, scaly patches on the skin. These patches can appear anywhere on the body but are most commonly found on the scalp, elbows, knees, and lower back.
Itching and burning
Psoriasis can be itchy and may cause a burning sensation, especially when the affected skin is exposed to water or other irritants.
Thickened and pitted nails
Psoriasis can also affect the nails, causing them to become thickened, discolored, and pitted. This can make it difficult to trim or manipulate the nails.
Joint pain and stiffness
In some cases, psoriasis can also affect the joints, causing pain, stiffness, and swelling. This is known as psoriatic arthritis and can be a severe form of the disease.
Dry and cracked skin
Psoriasis can cause the skin to become dry and cracked, which can make it more susceptible to infection.
Soreness and swelling
In some cases, psoriasis can cause soreness and swelling in the affected areas, which can make it difficult to move or perform daily activities.
Bleeding
In severe cases, psoriasis can cause the skin to crack and bleed, which can be painful and lead to infection.
While these are some of the most common signs and symptoms of psoriasis, it’s important to note that the severity and presentation of psoriasis can vary widely between individuals. If you are experiencing any of these symptoms, it is important to consult with a healthcare professional for proper diagnosis and treatment.
Types
Psoriasis is a chronic autoimmune skin condition that affects millions of people worldwide. There are several types of psoriasis, each with its own unique characteristics and symptoms. The most common types of psoriasis include:
Plaque psoriasis
This is the most common type of psoriasis, accounting for about 80-90% of all cases. It is characterized by raised, red, scaly patches that develop on the skin, usually on the scalp, elbows, knees, and lower back. These patches may be itchy and painful and can crack and bleed.
Guttate psoriasis
This type of psoriasis is characterized by small, red, drop-shaped lesions that appear on the arms, legs, and torso. It is most common in children and young adults and can be triggered by infections such as strep throat.
Inverse psoriasis
This type of psoriasis appears as smooth, red, inflamed patches in skin folds, such as the armpits, groin, and under the breasts. It can be particularly uncomfortable and painful because of its location.
Pustular psoriasis
This type of psoriasis is characterized by small, pus-filled blisters that develop on the skin. It can occur in small patches or cover large areas of the body. It is more common in adults and can be triggered by medications, infections, or stress.
Erythrodermic psoriasis
This is a rare but severe form of psoriasis that can cover the entire body. It causes red, inflamed skin that can be painful and itchy. It can also cause fever, chills, and other systemic symptoms.
Scalp psoriasis
This type of psoriasis affects the scalp and can cause red, scaly patches and flaking skin. It can be itchy and uncomfortable, and in severe cases, it can lead to hair loss.
Nail psoriasis
This type of psoriasis affects the nails, causing them to become discolored, thickened, and pitted. It can also cause the nails to separate from the nail bed.
Each type of psoriasis can have its own set of symptoms and treatment options, and people may have more than one type of psoriasis at the same time. It is important to work with a healthcare professional to develop an individualized treatment plan for managing psoriasis.
Treatment
There is currently no cure for psoriasis, but there are several medical treatments available that can help manage symptoms and reduce the frequency and severity of flare-ups. These treatments include topical medications, such as corticosteroids and vitamin D analogues, phototherapy, systemic medications, and biologic agents.
Topical medications are typically the first line of treatment for mild to moderate psoriasis. Corticosteroids are often used to reduce inflammation and itching, while vitamin D analogues can help slow down the growth of skin cells. Phototherapy, which involves exposing the skin to specific wavelengths of ultraviolet light, can also be effective in treating psoriasis.
For more severe cases of psoriasis, systemic medications and biologic agents may be necessary. These medications work by targeting specific components of the immune system to reduce inflammation and slow down the growth of skin cells. Some examples of systemic medications used to treat psoriasis include methotrexate, cyclosporine, and acitretin. Biologic agents, such as adalimumab, etanercept, and ustekinumab, work by targeting specific immune system proteins.
In addition to medical treatments, lifestyle changes can also be helpful in managing psoriasis. These changes may include avoiding triggers, such as stress and certain medications, maintaining a healthy weight, and getting regular exercise. Moisturizing the skin regularly and avoiding harsh soaps and detergents can also help reduce dryness and irritation.
Foods that can help
There are several types of foods that may help manage psoriasis symptoms in chronic autoimmune conditions. But note that these foods are not an alternative to medical treatment which may be required.
Fruits and vegetables: Fruits and vegetables are rich in antioxidants, vitamins, and minerals, which can help reduce inflammation and improve overall health. Dark leafy greens, berries, citrus fruits, and cruciferous vegetables, such as broccoli and kale, are particularly beneficial.
Fatty fish: Fatty fish, such as salmon, mackerel, and sardines, are rich in omega-3 fatty acids, which have anti-inflammatory properties. Consuming fatty fish or taking fish oil supplements may help reduce inflammation and improve psoriasis symptoms.
Nuts and seeds: Nuts and seeds are rich in healthy fats, such as omega-3 and omega-6 fatty acids, as well as vitamins and minerals. Examples include chia seeds, flaxseeds, almonds, and walnuts.
Turmeric: Turmeric contains curcumin, a compound that has anti-inflammatory properties. Consuming turmeric supplements or adding it to your diet can help reduce inflammation and psoriasis symptoms.
Probiotic-rich foods: Probiotics are beneficial bacteria that help support gut health. Consuming probiotic-rich foods, such as yogurt, kefir, sauerkraut, and kimchi, may help improve gut health and reduce inflammation.
Fiber-rich foods: Fiber is important for maintaining digestive health and reducing inflammation. Foods that are rich in fiber include whole grains, fruits, vegetables, legumes, and nuts.
It’s important to note that while these foods may help manage psoriasis symptoms, they should not be used as a replacement for prescribed treatments.
In conclusion, psoriasis is a chronic autoimmune condition that can have a significant impact on an individual’s quality of life. While there is currently no cure for psoriasis, there are several medical treatments available that can help manage symptoms and reduce the frequency and severity of flare-ups. In addition to medical treatments, lifestyle changes can also be helpful in managing psoriasis. If you think you may have psoriasis, it is important to consult with a dermatologist or healthcare professional for proper diagnosis and treatment.
References
Caiazzo G, Fabbrocini G, Di Caprio R, Raimondo A, Scala E, Balato N, Balato A. Psoriasis, Cardiovascular Events, and Biologics: Lights and Shadows. Front Immunol. 2018;9:1668.
Trayes KP, Savage K, Studdiford JS. Annular Lesions: Diagnosis and Treatment. Am Fam Physician. 2018 Sep 01;98(5).
Vázquez-Herrera NE, Sharma D, Aleid NM, Tosti A. Scalp Itch: A Systematic Review. Skin Appendage Disord. 2018 Aug;4(3):187-199.
Perez-Chada LM, Cohen JM, Gottlieb AB, Duffin KC, Garg A, Latella J, Armstrong AW, Ogdie A, Merola JF. Achieving international consensus on the assessment of psoriatic arthritis in psoriasis clinical trials: an International Dermatology Outcome Measures (IDEOM) initiative. Arch Dermatol Res. 2018 Nov;310(9):701-710.
Schadler ED, Ortel B, Mehlis SL. Biologics for the primary care physician: Review and treatment of psoriasis. Dis Mon. 2019 Mar;65(3):51-90.
This website does not provide medical advice.
All information provided on this website, and on associated social media networks, including but not limited to texts, images, and numbers are for general information purpose only. It is not intended as medical advice and it does not include all possible precautions, side effects, or interactions that may occur. Neither NaturalLivingOnline.com nor its author/founder take responsibility for how you use this information. Statements contained on NaturalLivingOnline.com have not been evaluated by the FDA. You should conduct thorough research via multiple sources and consult your physician or qualified doctor before using any essential oil or herbal remedy. Information on NaturalLivingOnline.com must not be relied upon for medical, legal, financial or other decisions.